A minor foot sore in a diabetic patient is often a ticking clock, but the real danger lies in misidentifying its origin. Is the underlying cause an arterial blockage or a venous failure? The wrong treatment path can lead to permanent damage. Uncover whether your diabetic ulcer is arterial or venous and why a Wound Care Specialist in Brooklyn, NY is essential for saving your mobility.
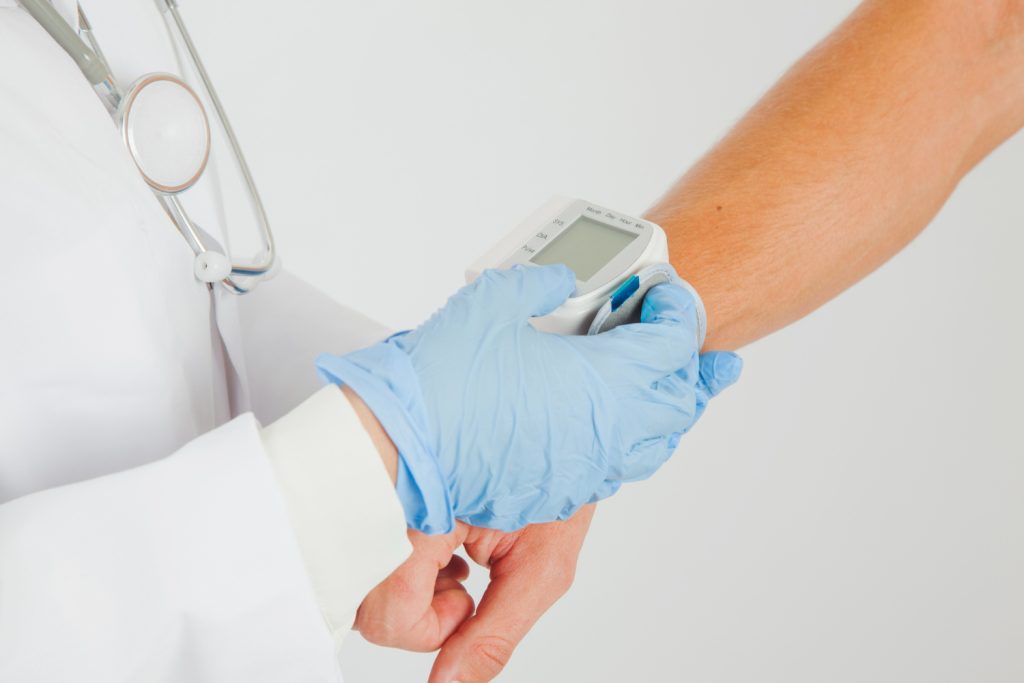
Advanced treatment Wound Care Specialist in Brooklyn, NY.
What Causes Diabetic Ulcers in the First Place?
Diabetic ulcers, particularly those affecting the feet, do not stem from a single cause but rather a complex combination of underlying conditions. The primary contributors are peripheral neuropathy, poor blood flow through arterial disease, and impaired healing, all of which are directly linked to long-term diabetes. Chronic high blood sugar damages both the nerves and blood vessels, creating an environment where injuries occur easily but heal remarkably slowly.
For example, nerve damage reduces the ability to feel pain, allowing minor cuts or pressure to go unnoticed, while reduced blood flow limits the oxygen and nutrients necessary for tissue repair. Clinical comprehension describes these ulcers as an interplay between vascular insufficiency, nerve damage, and a weakened immune response. Ultimately, these are not just simple skin wounds; they are the result of systemic changes in circulation and sensation caused by the disease.
Identify Blood Flow Problems From Arterial Disease
Peripheral arterial disease (PAD) is a leading factor in ulcer formation, occurring when arteries become narrowed or blocked. This restriction in blood flow prevents tissues from receiving adequate oxygen, making them highly vulnerable to breakdown.
- In diabetic patients, PAD frequently targets smaller, more distal blood vessels in the legs and feet.
- Even minor injuries can quickly progress into serious ulcers due to insufficient circulation.
- Ischemia, or lack of blood supply, significantly increases the likelihood of infection and tissue death.
- Without adequate perfusion, the body lacks the resources to effectively repair damaged skin.
- Arterial-related ulcers are recognized as being more severe and harder to treat than others.
Detect Venous Insufficiency and Poor Circulation
While arterial issues limit blood inflow, venous insufficiency affects the return of blood to the heart, leading to pooling in the lower limbs. This accumulation increases pressure within the tissues and reduces oxygen delivery, which directly contributes to skin breakdown.
| Condition | Primary Impact | Common Symptoms |
| Venous Insufficiency | Blood struggles to circulate efficiently, leading to pooling. | Chronic swelling and skin discoloration. |
| Poor Circulation | Creates an environment where skin becomes fragile and injury-prone. | Prolonged healing times and vulnerability in weight-bearing areas. |
Assess Nerve Damage From Long-Term Diabetes
Peripheral neuropathy is one of the most critical factors in the development of these wounds. Over time, high glucose levels damage the nerves, specifically in the feet, which leads to a significant loss of sensation. This loss of “protective sensation” means an individual may not feel the pain from a cut, blister, or constant pressure point.
Small, unnoticed injuries can worsen over time, leading to what research describes as “unnoticed repetitive injuries”. These repetitive traumas are a primary trigger for the formation of a chronic ulcer. Because the body’s natural warning system is compromised, the patient remains unaware that the tissue is being actively damaged.
Furthermore, neuropathy can physically alter the foot structure and the way a person walks, which increases pressure on specific areas of the foot. When combined with fragile, dry skin the risk of a complete skin breakdown and subsequent ulcer development rises sharply.
Recognize Pressure Points and Foot Trauma Risks
Mechanical stress, including friction and repeated trauma, plays a major role in the formation of diabetic ulcers. In patients with neuropathy, these stress points are particularly dangerous because the discomfort is not felt.
- Continuous pressure on the soles of the feet can lead to callus formation and skin thickening.
- Foot deformities and improper footwear further increase localized pressure during movement.
- Abnormal walking patterns can create micro-injuries that evolve into chronic, non-healing wounds.
- Regular foot inspections are essential because everyday activities like walking can trigger these hidden injuries.
Evaluate Infection and Delayed Wound Healing Factors
Once a wound has formed, impaired immune function and high blood glucose levels interfere with the body’s natural inflammatory response and tissue repair processes. This results in delayed healing, allowing wounds to persist for months. Infections are common because damaged tissue and poor circulation create an ideal environment for bacteria to thrive.
If not treated promptly, these infections can spread to deeper tissues, leading to severe complications like bone infections or the need for amputation. Effective treatment requires a comprehensive approach that addresses the overlapping issues of blood flow, nerve damage, and metabolic imbalance.
Key Takeaways.
- Complex Systemic Causes Diabetic ulcers develop from a complex interplay of nerve damage, poor blood flow, and weakened immune responses. Chronic high blood sugar damages both vessels and nerves, allowing injuries to occur easily while healing progresses slowly.
- Arterial vs. Venous Insufficiency Arterial disease restricts oxygen inflow through blocked vessels, causing severe ischemia and a high risk of tissue death. Conversely, venous insufficiency causes blood to pool in the limbs, increasing tissue pressure and reducing oxygen delivery.
- Impact of Peripheral Neuropathy Nerve damage creates a loss of “protective sensation,” meaning patients often cannot feel pain from cuts or blisters. This leads to repetitive, unnoticed injuries that serve as the primary triggers for chronic ulcer formation.
- Mechanical Stress and Pressure Points Repeated mechanical stress from friction or improper footwear can damage the soft tissue on the soles of the feet. Continuous pressure leads to dangerous callus formation and skin thickening that often evolves into a chronic wound.
- Infection and Healing Complications Impaired immune function and high glucose levels interfere with the body’s natural ability to fight bacteria and repair tissue. If not treated promptly, infections can spread to deeper tissues, leading to severe complications like bone infections or amputation.
FAQs:
Is diabetic ulcer arterial or venous?
A diabetic ulcer is typically not just one or the other; it develops from a complex combination of conditions. While peripheral arterial disease (arterial) is a main contributor, venous insufficiency can also coexist with diabetic complications.
Are ulcers arterial or venous?
Ulcers can be either arterial or venous. Arterial ulcers are caused by narrowed or blocked arteries that reduce oxygen delivery to tissues, while venous ulcers result from veins struggling to return blood to the heart, causing pooling in the limbs.
What is the difference between an arterial ulcer and a diabetic ulcer?
An arterial ulcer is caused specifically by peripheral arterial disease (PAD). A diabetic ulcer is a systemic wound caused by multiple overlapping issues, including not only arterial disease but also peripheral neuropathy (nerve damage) and impaired immune function.
Is diabetic wound vascular?
Yes, a diabetic wound has a major vascular component. These ulcers are the result of systemic changes in circulation and vascular insufficiency caused by diabetes, which limits the oxygen and nutrients necessary for tissue repair.
Sources.
Marco, M., Valentina, I., Daniele, M., Valerio, D. R., Andrea, P., Roberto, G., Laura, G., & Luigi, U. (2021). Peripheral Arterial Disease in Persons with Diabetic Foot Ulceration: a Current Comprehensive Overview. Current diabetes reviews, 17(4), 474–485. https://doi.org/10.2174/15733998169992010012 03111
Aditya, C., Bukke, S. P. N., Anitha, K., Meeraraje, P., Goruntla, N., Yadesa, T. M., & Onohuean, H. (2025). A comprehensive review on diabetic foot ulcer addressing vascular insufficiency, impaired immune response, and delayed wound healing mechanisms. Frontiers in pharmacology, 16, 1622055. https://doi.org/10.3389/fphar.2025.1622055
You May Also Like:
How Often Should a Diabetic See an Endocrinologist?
How Often Should You See an Internist for Regular Check- …
Allhealth in Coney Island Avenue
1100 Coney Island Avenue,
2nd Floor, Brooklyn, NY 11230
Phone: (718) 942-4944
Email: IDD@allhealthdtc.com
Allhealth in East 13th Street
1655 East 13th Street,
Brooklyn, NY 11229
Phone: (718) 339-6900
Email: medical@allhealthdtc.com

